Scientists Link
|
|
 Nutritional biochemist Elizabeth Johnson uses high-performance liquid chromatography to measure carotenoids in blood plasma. Carotenoids play a role in the prevention of age-related cataracts. Because carotenoids break down under normal room light, a red light is used for illumination during the test. (K10510-1) |
About 16 million people in the United States over age 45 report some vision loss. This group may find hope in a growing body of evidence that diet can influence eye health. ARS has several scientists studying the possibility of reducing—by way of dietary modification—the risk of two common sight-robbing disorders: cataract formation and age-related macular degeneration. About 20 years ago, scientists were hard-pressed to find published research studies on correlations between nutrition and risk of eye disease. But steady efforts by government and academic researchers over the years have led to a clearly established discipline of ophthalmologic nutrition and epidemiology. A Cloudy Matter For baby boomers reaching an age at which steady vision can no longer be taken for granted, many are wishing they'd worn sunglasses when young. Sunlight is somewhat of a natural enemy to the eye's lens. |
 Dietitian Helen Rasmussen weighs exact amounts of lutein-enriched eggs and other ingredients for an egg frittata that participants will eat during testing to see whether food type affects lutein absorption into the bloodstream. (K10508-5) |
"Lens cells make a specific, predominant set of proteins called crystallins," says bio-organic chemist Allen Taylor. He is chief of the Laboratory for Nutrition and Vision Research at the Jean Mayer USDA Human Nutrition Research Center on Aging (HNRCA) at Tufts University in Boston, Massachusetts. "Those proteins act like fiber optics, allowing light to pass through the lens and onto the retina," he says. They must function over decades with little opportunity for repair. Red, blue, green, yellow, and ultraviolet (UV) wavelengths penetrate the transparent lens. But UV light appears to be particularly damaging to the lens, and blue light appears to damage the retina—a complex, sensory membrane that lines the eye and receives the images formed by the lens. Normal byproducts of metabolism, called oxygen free radicals, also cause damage. If not neutralized by an antioxidant, over time such oxidation damages the lipids, proteins, and other components of the lens. The result is a clouding of the lens in a gradual slide from transparent to opaque. These opacities are called cataracts. Antioxidants are compounds in foods that help maintain healthy cells and tissues in the eye and other organs. Inside the lens are high levels of vitamins C and E as well as some lutein and zeaxanthin. The latter two fall within a class of phytochemicals called carotenoids, and they are concentrated in the retina. |
 Chemist Allen Taylor as seen through rat's eye lenses with cataracts (left) and without (right). Note that Taylor's face is fuzzy in the image on the left but clear on the right. (K10597-28) |
"As damaged proteins gather, they result in lens opacities," says Taylor. His research suggests that protective, antioxidant-rich nutrition could be the least costly and most practical means to delay cataracts. "The accumulation of oxidized or modified proteins we've observed is consistent with the failure of protective systems to keep pace with the insults that damage lens proteins," he says. The protective systems include protein-digesting enzymes, which may seek out and destroy damaged proteins, as well as antioxidants, which can lessen initial damage and may keep protective enzymes functioning longer. In economic and human terms, damage to lens proteins is costly. About half of those over 75 in the United States will experience a visually significant cataract. The costs of cataract-related disability and cataract surgery now total $6 billion annually worldwide. |
 Chemist Allen Taylor and technician Marisa Hobbs examine parts of an eye lens grown in a petri dish to determine what happens during lens aging and cataract formation. (K10509-15) |
Various Causes Three distinguishable areas of the lens can be affected by cataracts: the nuclear, cortical, and posterior subcapsular (PSC) areas. The nuclear and cortical areas are associated with age-related cataracts, while the PSC area is associated with diabetes-related cataracts. Nuclear lens opacity has been the most widely studied of the three lens areas. Paul F. Jacques, Taylor, and colleagues reported in 2001 that antioxidant nutrients play a role in the prevention of nuclear cataracts. Jacques is chief of HNRCA's Nutritional Epidemiology Program. The scientists looked at 478 nondiabetic women from Boston, aged 53 to 73 years and not previously diagnosed with cataracts. These women were sampled from the Nutrition and Vision Project (NVP), a substudy of the federally funded Nurses' Health Study. Researchers conducted eye exams to study the relationship between newly diagnosed nuclear opacities and nutrient intake over time. Food intake was assessed from multiple food frequency questionnaires completed over 13 to 15 years. |
 Nutritional biochemist Elizabeth Johnson extracts lipids from blood plasma to test for carotenoids. (K10511-9) |
The study showed that women with the highest intakes of vitamins C and E, riboflavin, folate, beta carotene, lutein, and zeaxanthin had a lower prevalence of nuclear opacification than did those with the lowest intakes of those nutrients. Moreover, those who used vitamin C supplements for 10 or more years were 64 percent less likely to have nuclear opacification than those who never used vitamin C supplements. Taylor, Jacques, and colleagues reported similar findings in 2002 when they looked for cataracts in the cortical and PSC regions of the lens in some NVP participants. Those findings support a role for vitamin C in reducing the risk of cortical cataracts in women younger than 60. The data also indicated that women who consumed higher amounts of carotenoids had a lower risk of PSC cataracts if they had never smoked. In the same NVP population, women who regularly took vitamin E had less progression of eye lens damage, as Taylor reported during last year's Association for Research in Vision and Ophthalmology proceedings in Fort Lauderdale, Florida. "The increase in nuclear opacification—over 5 years of follow-up after their initial examination—was 30 percent lower among women who used vitamin E supplements for at least 10 years than among those who had never used vitamin E supplements," says Jacques. |
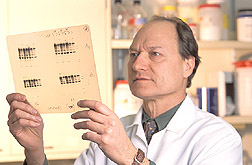 Chemist Allen Taylor views films that show that oxidative stress damages eye lens proteins. (K10506-5) |
Another recently completed study explored the relationship between body mass index, waist circumference, diabetes, and the presence of age-related cataracts in women. The study supports other findings that diabetes is a strong risk factor for PSC opacities and that abdominal fat and obesity may also be associated with PSC.Several variables complicate a comprehensive evaluation of the existing evidence linking nutrition and age-related vision loss. "Definitions of cataract may differ from one study to another, and the various methods for assessing the intake or status of nutrients, such as antioxidants, certainly complicate matters," says Jacques. "There are several questions that still need to be resolved." At this point, what scientists do know is that oxidative damage within the eye is harmful to several eye tissues. The Yellow Spot Among Americans who are 55 or older, age-related macular degeneration (AMD) is reported to be a leading cause of blindness and vision impairment. According to the National Eye Institute (NEI), more than 1.6 million Americans in that age group have advanced AMD. Some experts estimate up to 7 million more may be at the intermediate stage. They see fine now, but they are at high risk for developing the advanced form, which causes vision loss. Among the causes of AMD, scientists describe a breakdown of light-sensitive cells within the retina. The focus is on a 3-millimeter-wide yellow spot, called the macula lutea, toward the back and center of the eye. The macula plays a key role in the central part of visual images. But as the eye ages, oxidized proteins, or debris called drusen, begin to pile up and cause trouble. Taylor and other scientists are seeking to unravel the mystery of why this process happens. Scientists have long known that the yellow color, or pigment, inside the macula comes from the carotenoids lutein and zeaxanthin. Many scientists believe that these plant chemicals help protect the eye by absorbing blue light and neutralizing free radicals. But as the body ages, the importance of carotenoids in the macula may increase because of the lifelong exposure to damaging light. These two carotenoids circulate in the food supply and in blood plasma at a ratio of about one part zeaxanthin to about six or seven parts lutein. As blood passes by the macula through retinal blood vessels, these pigments pass through the macula's outer layer to rest in high concentrations inside its center. Perhaps most interesting is that people with macular degeneration have been found to have lower levels of zeaxanthin and lutein in the macula than people without—which supports the premise that these antioxidants provide some protection. Absorbing Research Nutritional biochemist Elizabeth J. Johnson, who is with HNRCA's Carotenoids and Health Laboratory, is now leading a study aimed at determining differences in the body's absorption and use—known as bioavailability—of lutein from eggs, spinach, and supplements. After study volunteers—healthy adult men—consumed cooked spinach, eggs, and lutein supplements, Johnson measured levels of lutein and triglyceride-rich lipoproteins in their blood serum. The study, which is supported by the Egg Nutrition Center, in Washington, D.C., used eggs from chickens that had been fed marigold petals, which are high in lutein. Consumption of these eggs considerably increased the lutein in volunteers' blood. "After volunteers ate eggs as a source of lutein, their blood serum level of lutein was two to three times greater than it was after they ate the same amount of lutein from other sources," says Johnson. These preliminary results provide compelling evidence that eggs can be a more bioavailable source of lutein than more conventional sources, such as spinach and supplements. "We don't know why the lutein in egg yolks is more bioavailable, but we think it's due to other components in the yolks, such as lecithins." The "designer" eggs used in the study had about six times—about 1.5 milligrams—the lutein of standard eggs. Still, spinach has about 11 milligrams per 2-ounce serving. "Even though the lutein in the eggs is a comparatively tiny amount, it goes right into the bloodstream," says Johnson. She has also studied and will soon report the effects of lutein and zeaxanthin supplementation on carotenoid levels in the blood, adipose (fat) tissue, and macula of monkeys. That research has led to new findings about the source of an important form of zeaxanthin, called meso zeaxanthin. Curiously, that form is found in the macula, but not in food or blood. It may be better than lutein at reducing damage from light entering the eye. Johnson believes meso zeaxanthin could actually be formed from lutein once it's inside the macula itself. Diminishing Risk In 2001, NEI researchers reported results from the 7-year Age-Related Eye Disease Study, or AREDS. Results showed that people lowered their risk of developing advanced AMD by about 25 percent when they took a high-dose combination of vitamins C and E, beta-carotene, and zinc for more than 6 years. NEI defines high risk as having intermediate or advanced AMD in one eye. In those with advanced AMD, the nutrients reduced their risk of further vision loss by about 19 percent. NEI concluded that while the nutrients will not restore vision already lost from the disease, they may play a key role in helping high-risk people keep their remaining vision. Lutein supplements were not available at the study's inception, but NEI is starting to study it now. "Lutein is compelling because of evidence that it neutralizes free radicals," says Johnson. "Since it's in the macula, it's right where it needs to be to protect against damage." In the meantime, during regular examinations, eye doctors can see the telltale signs of early, intermediate, and advanced AMD. The AREDS supplements had no significant effect on cataract development or progression. But intervention was only for about 6 years, and some people in the control group had already taken, or continued to take, antioxidant supplements. Cataract surgery is the most expensive outpatient surgery covered by Medicare. While some see surgery as a stopgap intervention for cataracts, there is as yet no known surgical remedy for AMD, making optimal nutrition all the more attractive. Researchers focusing on eye health today agree that for some, nutrition will play an important role in lessening the risk of developing these sight-robbing eye disorders.—By Rosalie Marion Bliss, Agricultural Research Service Information Staff. This research is part of Human Nutrition, an ARS National Program (#107) described on the World Wide Web at www.nps.ars.usda.gov. To reach scientists mentioned in this article, contact Rosalie Bliss, USDA-ARS Information Staff, 5601 Sunnyside Ave., Beltsville, MD 20705; phone (301) 504-4318; fax (301) 504-1641. "Scientists Link Nutrition & Eye Health" was published in the August 2003 issue of Agricultural Research magazine.
|






