Arthritis From Foodborne Bacteria?
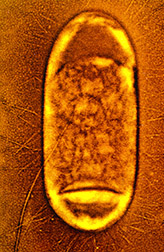 This Salmonella typhimurium bacterium is about half a micrometer (millionth of a meter) wide. (K7482-1) |
People who have had bacterial food poisoning may have potential for illness other than just the temporary inconvenience of diarrhea and vomiting.
"Certain individuals may suffer chronic joint diseases, such as reactive arthritis, after being infected with bacteria ingested with food," says James L. Smith.
Smith, who is retired from ARS' Eastern Regional Research Center at Wyndmoor, Pennsylvania, has been studying the relationship between foodborne bacteria and arthritis. Now a collaborator and microbiologist emeritus associated with the center's Microbial Food Safety Research Unit, he has come up with some fascinating findings.
Infections from four rather common foodborne pathogens'Campylobacter, Salmonella, Shigella, or Yersinia—may lead to reactive arthritis, he says.
"When we think of bacterially induced arthritis, it's usually the septic type in which the infecting organism is present in the joint," says Smith. "As it grows there, it can cause inflammation and destruction of joint tissue.
"In sterile, or reactive, arthritis, organisms are not present in the joint. Antigenic components of the infecting bacteria are there, but viable, living organisms are not," Smith explains.
It is interesting, he says, that an infection in the gastrointestinal tract by Campylobacter, Salmonella, Shigella, or Yersinia bacteria can somehow lead to inflammation of an organ or joint that is far removed from the site of infection.
"Genetic makeup may predispose individuals to reactive arthritis," Smith says. "No one knows why, but individuals carrying the gene responsible for producing the human leucocyte antigen HLA-B27 are more susceptible to arthritis.
"We do know that the molecular structure of antigens from these particular foodborne bacteria mimic the HLA antigen. It has been suggested that this antigen mimicry could be a mechanism for causing arthritis."
An antigen is a substance that, when introduced into the body, causes the body to produce antibodies to fight the foreign substance and create immunity to it. Antigens can be toxins, bacteria, viruses, or foreign blood cells. T-cells are immune cells that activate other cells that directly destroy pathogens.
The HLA-B27 gene is found in about 10 percent of healthy Caucasians, 1 percent of Japanese, and up to 4 percent of North American blacks but is absent from African and Australian blacks. While only about 2 percent of the people who get food poisoning develop arthritis, about 20 percent of those exposed who have the HLA-B27 gene get it.
Smith cites a recent outbreak of milkborne salmonellosis in the United States that made about 198,000 people ill. After that infection, arthritis was found in about 2.3 percent—more than 4,500—of those actually infected with the bacteria.
Foods that can carry Campylobacter, Salmonella, Shigella, or Yersinia bacteria include raw and undercooked meat, poultry, eggs, shellfish and other seafood, unpasteurized milk, fruit, and vegetables. Untreated drinking water and household pets are also sources.
Although they are the most commonly reported, bacterially caused foodborne illnesses are the easiest to prevent. To kill bacteria, consumers should always cook foods (especially meat, poultry, and eggs) thoroughly, keep raw and cooked foods separate, and promptly refrigerate cooked foods in shallow containers. Raw fruits and vegetables should be washed with water.
"For most people, an infection from foodborne bacteria just means feeling rotten for a day or so. But for an unfortunate few, it can mean the severe hardship of arthritis," Smith says. -- By Doris Stanley, ARS.
James L. Smith can be reached at the USDA-ARS Microbial Food Safety Research Unit, Eastern Regional Research Center, 600 East Mermaid Lane, Wyndmoor, PA 19038-8551; (215) 233-6520.
"Arthritis From Foodborne Bacteria?" was published in the October 1996 issue of Agricultural Research magazine.






